
Specialties:
Sports Injuries, Badminton-Related Injuries, Concussion, Musculoskeletal Injuries, Frozen Shoulder, Shoulder Pain, Arthritis, Degenerative Joint Disease, Low Back Pain, Cervical Disc Herniation, Lumbar Disc Herniation, Exercise Prescription, Exercise Recommendations for Older Adults and Special Populations, Prolotherapy, Regenerative Medicine, Platelet-Rich Plasma (PRP) Injections, Ultrasound-Guided Injections, and X-ray–Guided Injections.
Radiofrequency
Treatment — A New Option for Back Pain Relief
Lower back pain is extremely common, affecting up to 80% of
people at some point in their lives. One of the common causes is a herniated
lumbar disc, which may compress the spinal nerves. Besides back pain,
patients often experience leg symptoms such as aching, tightness, numbness,
tingling, or sharp pain, commonly known as sciatica. Herniated discs
occur most frequently between the ages of 20 and 50, but may also happen
in elderly, which are associated with prolonged sitting, poor posture, heavy
lifting, and sports injuries.
Conventional treatments include rest, medication, physical therapy,
and—when necessary—steroid nerve root injections. In the past, patients
with persistent or worsening symptoms often needed surgery to decompress the
nerve. However, it is important to note that imaging findings do not always
match symptoms. Some people show significant disc herniation on MRI yet
have no pain, while others experience severe pain without major imaging
changes. This means an abnormal MRI does not automatically require surgery,
and many patients improve through reinforced conservative care.
However, if red flags appear—such as loss of bladder or bowel
control, sudden leg weakness, fever with possible severe infection, or
neurological symptoms after a major injury—urgent surgical evaluation is
required to avoid delayed treatment.
For patients without these emergency conditions, radiofrequency (RF)
treatment has become a promising, minimally invasive alternative in recent
years.
What Is Radiofrequency Therapy?
Radiofrequency (RF) therapy is a minimally invasive procedure that
uses a special needle and electrical stimulation to reduce nerve
hypersensitivity. Think of it this way: when a child falls and feels pain, an
adult might gently blow on the injured area to soothe it. RF therapy works
similarly—it “calms down” the irritated nerve so it stops sending
excessive pain signals.
There are two main types:
1.
Conventional Radiofrequency Ablation (RFA)
Uses high temperature to deactivate sensory nerves and provide pain
relief.
2. Pulsed
Radiofrequency (Pulsed RF)
Operates at a lower temperature (~42°C), does not burn or destroy
the nerve, and mainly reduces pain by regulating nerve excitability and
preventing the amplification of pain signals.
Studies show that for chronic nerve pain lasting more than three
months, pulsed RF often provides longer-lasting relief compared to
traditional injections alone.
RF can also be combined with regenerative treatments such as platelet-rich
plasma (PRP) to support nerve healing, with some patients experiencing
better outcomes than steroid injections.
How Is Radiofrequency Therapy Performed?
Your doctor will first conduct a detailed interview, physical
examination, and imaging review (such as X-ray or MRI) to confirm that the pain
is truly related to nerve compression.
Because the spine is surrounded by bone and ultrasound cannot
penetrate bone structures, the procedure requires X-ray guidance and
contrast dye to accurately reach the nerve. Therefore, RF treatment is
performed in medical facilities equipped with appropriate imaging technology.
Procedure
Overview
- Patients
taking anticoagulants may need to discuss temporary discontinuation to
reduce bleeding risk.
- Most
patients lie face-down during the procedure.
- Depending
on the number of nerves treated, the entire procedure takes 30–60
minutes.
- It is an outpatient
procedure. Only a tiny puncture is required, hospitalization is not
needed, and patients can go home after a brief observation period.
Most patients can walk normally afterward. A small number may
experience temporary soreness or numbness, which usually improves within a few
days.
Who Is a Good Candidate for Radiofrequency Treatment?
How Long Does the Relief Last?**
RF therapy may be suitable for patients with:
- Confirmed
sciatica caused by nerve root compression
- Limited
improvement from medication, physical therapy, or traditional injections
- A desire
to reduce or delay the need for surgery
- Medical
conditions that make surgery higher risk (elderly patients, multiple
comorbidities, anesthesia concerns)
The duration of pain relief varies by individual and depends on
factors such as degree of nerve compression, lifestyle habits, and muscle
condition.
A helpful analogy:
Even if a professional cleaning service tidies up your home, it will
become messy again quickly if things are thrown around the next day.
RF therapy can reduce your pain, but long-term improvement depends heavily on
your own habits — posture correction, reducing long sitting time, and regular
core muscle training.
Active rehabilitation is strongly recommended to maintain the
benefits, rather than relying solely on passive treatments.
Summary
Although herniated discs and sciatica can be frustrating, not all
patients require surgery. Only those with urgent warning signs or
progressive neurological deficits should prioritize surgical treatment. For
many patients with recurrent symptoms that have not yet reached the
threshold for surgery, radiofrequency therapy is a safe, effective, and
fast-recovery option, often considered the final step before surgical
intervention.
If you are experiencing lower back pain or sciatica, we encourage
you to consult with a medical professional to determine the most appropriate
treatment—so you can restore your comfort and improve your quality of life as
soon as possible.
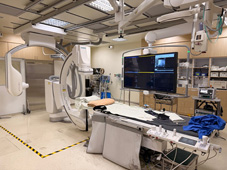
Advanced
biplane fluoroscopy (dual-plane X-ray) to perform highly precise image-guided
injections
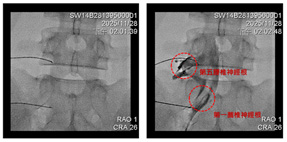
After
guiding the needle to the correct location under X-ray, contrast is used for
confirmation before performing the targeted treatment

The interdisciplinary pain management team
at Far Eastern Memorial Hospital (second from the left, Dr. Wei-Ting Lin;
center, Dr. Yu-Ping Huang; and radiologic technologists and nursing staff).